A. Gironés Muriel.
Adjunto al Servicio de Anestesia del Hospital Sanitas La Moraleja.
P. Serrano Marcos
DUE Servicio Quirúrgico del Hospital Sanitas La Moraleja.
Artículo Original: Use of face masks by non-scrubbed operating room staff: a randomized controlled trial Webster J. Et al. ANZ J Surg 2010 Mar; 80 (3) (PubMed)
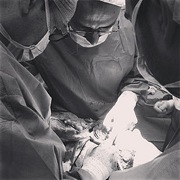
Sin entrar en discusiones bizantinas, es bueno pararse a pensar en la evidencia encontrada para dicha afirmación. Aparte de encontrar múltiples recomendaciones y protocolos que obligan a ponerse la mascarilla facial al entrar en quirófano, convirtiéndose en un ritual asimilado por todos, sorprendentemente no existen muchos estudios con un nivel adecuado que sostengan tal afirmación.
Debemos pensar que las barreras de protección son un método sencillo y barato de disminuir al máximo la tasa de infección postoperatoria y, por tal motivo, los autores no van a ser unos reaccionarios en este tema. Sin embargo, no está de más hacer una revisión crítica sobre la cuestión a través del método empírico y los niveles de evidencia que tan buenos resultados ha dado a nuestra profesión.
La Cochrane se hizo eco de tal asunto con un metaanálisis sobre la implicación de la mascarilla facial en la infección postquirúrgica durante la llamada cirugía limpia, publicado en 2.002. Exponemos aquí alguna de sus conclusiones.
Disposable surgical face mask for preventing surgical wound infection in clean surgery. Lipp A , Edwards P. Cochrane database syst rev 2.002 (PubMed) (Cochrane web)
- Existen pruebas insuficientes que apoyen el uso de las mascarillas desechables para prevenir el uso de la mascarilla facial en la cirugía limpia.
- El diseño de las mascarillas actuales puede, según autores, incrementar la contaminación postquirúrgica, ya sea por el efecto de“ escape lateral“, por efecto“ mecha“ o capilaridad, (wicking) o por efecto serpenteo (wiggling), al descamar la mascarilla la cara del usuario por fricción y dispersar dichas escamas por el quirófano.
- Sólo se encontraron 2 estudios aleatorizados controlados para la revisión de los 13 estudiados. De ellos, 1 fue abandonado por la aparición de infecciones postquirúrgicas que no podían deberse al personal presente en la intervención.
- Existen sesgos potenciales y limitaciones de diseño en todos los estudios recogidos.
- Por ello, la conclusión de los autores es que, por resultados limitados, no pueden afirmar que el uso de mascarillas faciales causa daño o beneficio al paciente sometido a cirugía limpia.
Pero, aparte de este metaanálisis realizado por la Cochrane, existen bastantes evidencias que van en contra de este ritual tan familiar consistente en colocarse la mascarilla facial para entrar en un quirófano. Ya en el siglo pasado, editoriales como el de The Journal of Bone and Joint Surgery por S.P.F Hughes afirmaban contundentemente que no existían evidencias que sugiriesen que colocarse la mascarilla facial fuera del área de operación supusiera un beneficio[1]. En la revista Journal Hospital Infections de 1.991, Mitchell N.J y col. lo afirmaron con más vehemencia[2]. Pero, por más actual, nos llama la atención un artículo de 2.010 aleatorizado que tiene la misma opinión, realizado por compañeros no médicos (enfermeros) con una calidad de diseño que muchas veces echamos en falta en los estudios diseñados por colegas médicos.
Use of jace mask by no-scrubbed operating room staff; a randomized controlled trial. Por Webster J y colaboradores publicado en el ANZ Journal of Surgery 80 (3).
Un estudio de un nivel más que aceptable, con una puntuación de 3 en la escala Jadad, con una aleatorización, descripción de seguimientos y pérdidas a nuestro entender correcto. Prospectivamente siguieron a 827 pacientes destinados a operarse distribuidos aleatoriamente en 2 quirófanos. Uno, donde todo el personal llevaba puesta la mascarilla facial, y otro en la que sólo la llevaba el personal“ estéril“. Se controlaron y anotaron múltiples factores que pudiesen interferir en la aparición de la infección: estado físico del paciente, tiempo de cirugía, clasificación de la herida, índice de masa corporal, historia de infección previa, profilaxis antibiótica, tipo de cirugía, número de personas en quirófano, presencia de hábitos tóxicos. Siguieron a los pacientes aproximadamente 1 mes para confirmar la presencia o no de infección en la herida quirúrgica, mediante una nominalización y clasificación, también correcta.
El tipo de cirugía fue variado, aunque el 81% fue de tipo CMA.
Datos obtenidos
El 10,2% de los pacientes tuvieron infección. El 11,5% en el grupo con mascarilla facial y 9,5% en el grupo sin mascarilla. Una diferencia no estadísticamente significativa con un OR de 0,77 (CI 95% 0,49-1,21 con p=0,15). Sólo en el 31% de las infecciones fue identificado el agente patógeno (principalmente stafilococo aureus).
Con una regresión logística concluyeron que los factores implicados en la infección de la herida quirúrgica fueron:
1.- La presencia de hospitalización.
2.- Un alto índice de masa corporal (IMC)
3.- Tener antecedentes de infección de la herida quirúrgica.
Conclusión
Este y otros artículos al respecto nos llevan a ser cautos al respecto. A nuestro entender los datos sugieren que el uso de la mascarilla es mucho menos importante de lo que la gente cree a simple vista… pudiendo ser innecesario su uso fuera del campo quirúrgico.
Pero eso no quita para usarla siempre en contextos de alta probabilidad de infección o en situaciones en las que el sentido común pueda primar por encima de estos datos estadísticos.
Una cosa es la verdad estadística y otra la verdad clínica, si bien, la primera es una buena manera de encontrar la segunda.
Bibliografia
[1]SPF Hughes et al. Infection in the operating room (editorial) Journal of Bone an Joint Surgery 1.999 (PubMed) (pdf)
[2] Mitchell NJ et al. Surgical face mask in modern operating rooms: a costly and unnecessary ritual?. J.Hospital Infecc 1.991; 18. 811-3 (PubMed)




Hola a todos!
Este artículo me ha sorprendido pero tengo una mente muy abierta a la evolución dentro de nuestro campo profesional y sinceramente, si llegase el día en que las organizaciones oficiales reconocidas mundialmente (AORN, ASA, OMS…..) recomendasen el «no uso» de la mascarilla quirúrgica por parte de los miembros del equipo «no estéril», yo sería feliz, me quitaría de encima una lucha diaria para que se use la mascarilla dentro del quirófano, siempre que hay materiales estériles abiertos, como recomienda la AORN en su publicación de este año, recomendaciones que compro y estudio para estar actualizada. Para el que tenga interés en adquirir alguna de las recomendaciones y de forma individual, os pongo el enlace donde podéis comprarlas:
<a href="http://webstore.ansi.org/FindStandards.aspx?SearchString=AORN&SearchOption=0&DeptID=&PageNum=3&SearchTermsArray=null%7cAORN%7cnull" rel="nofollow ugc">http://webstore.ansi.org/FindStandards.aspx?SearchString=AORN&SearchOption=0&DeptID=&PageNum=3&SearchTermsArray=null%7cAORN%7cnull</a>
En cualquier caso y aunque este comentario se haga un poco extenso, os voy a copiar una pequeña parte de la recomendación de la Técnica Estéril, de este año y en la cual se desarrolla la recomendación del uso de la mascarilla quirúrgica basada en linvestigaciones:
RECOMMENDED PRACTICES FOR STERILE TECHNIQUE
Purpose
These recommended practices provide guidance for establishing and maintaining a sterile field by following the principles and implementing the processes of sterile technique. Sterile technique involves the use of specific actions and activities to prevent contamination and maintain sterility of identified areas during operative and other invasive procedures. Implementing sterile technique when preparing, performing, or assisting with surgical and other invasive procedures is the cornerstone of maintaining sterility and preventing microbial contamination.
The creation and maintenance of a sterile field can directly influence patient outcomes.1 All individuals who are involved in operative or other invasive procedures have a responsibility to provide a safe environment for patients. Perioperative team members must be vigilant in safeguarding the sterility of the field and ensuring that the principles and processes of sterile technique are followed and implemented. Perioperative leaders can promote a culture of safety by creating an environment where perioperative personnel are encouraged to identify, question, or stop practices believed to be unsafe without fear of repercussion.
Evidence Review
A medical librarian conducted a systematic review of MEDLINE®, CINAHL®, Scopus®, and the Cochrane Database of Systematic Reviews for meta-analyses, randomized and nonrandomized trials and studies, systematic and nonsystematic reviews, and opinion documents and letters. Search terms included sterile field, sterile technique, aseptic technique, aseptic practices, surgical drapes, double-gloving, assisted gloving, closed gloving, time-related sterilization, event-related sterilization, surgical attire, protective clothing, sterile supplies, sterile barriers, barrier precautions, body-exhaust suits, space suits, laminar air flow, bowel technique, (glove expansion and fluids), (glove perforation and electrosurgery), strikethrough, Spaulding»™s criteria, product packaging, and equipment contamination.
The lead author and medical librarian identified and obtained relevant guidelines from government agencies, other professional organizations, and standards-setting bodies. The lead author assessed additional professional literature, including some that initially appeared in other articles provided to the author.
The initial search was confined to 2006 to 2011, but the time restriction was not considered in subsequent searches. The librarian also established continuing alerts on the topics included in this recommended practice and provided relevant results to the lead author.
Articles identified by the search were provided to the project team for evaluation. The team consisted of the lead author, two members of the Recommended Practices Advisory Board, and a member of the Research Committee. The lead author divided the search results into topics and assigned members of the team to review and critically appraise each article using the Johns Hopkins Evidence-Based Practice Model and the Research or Non-Research Evidence Appraisal Tools as appropriate. The literature was independently evaluated and appraised according to the strength and quality of the evidence. Each article was then assigned an appraisal score as agreed upon by consensus of the team. The appraisal score is noted in brackets after each reference, as applicable.
Recommendation I
Perioperative personnel should implement practices that reduce the spread of transmissible infections when preparing or working in the OR or invasive procedure room and when performing or assisting with operative or other invasive procedures.
Protecting patients and safeguarding health care providers from potentially infectious agent transmission is a key focus of perioperative nurses.5 Hand hygiene has been recognized as a primary method of decreasing health care-associated infections.4,6 Surgical attire and personal protective equipment (PPE) are worn to support cleanliness and hygiene, promote patient and health care provider safety, and aid in preserving the integrity of the sterile field within the perioperative environment.3,5
«¢ I.a. Perioperative personnel entering the OR or invasive procedure room for any reason (eg, stocking supplies, bringing procedural supplies and equipment into clean rooms) should wear clean
o â—‹ scrub attire,1 including a freshly laundered or single-use, long-sleeved jacket snapped closed with the cuffs down to the wrists, and
o â—‹ surgical head covers or hoods that cover all hair and scalp skin, including facial hair, sideburns, and the hair at the nape of the neck.1
[Recommended for Practice]
Surgical attire helps contain bacterial shedding and promotes environmental cleanliness.1,3Head coverings and hoods minimize microbial dispersal by containing hair and scalp skin.1,3
«¢ I.b. Perioperative personnel should perform hand hygiene before entering the OR or invasive procedure room and areas where sterile supplies have been opened. [Recommended for Practice]
Following regular hand hygiene practices helps prevent transmission of infection and reduces health care-associated infections for patients and health care personnel.4,6
Prevention of health care-associated infections is a priority of all health care providers. Health care-associated infections can result in untoward outcomes such as increased morbidity and mortality, longer length of stay, increased pain and suffering, and escalating cost of care.7Hand hygiene, hand washing, and surgical hand scrubs are the most effective way to prevent and control infections and represent the least expensive means of achieving both.4
«¢ I.c. Perioperative personnel should wear a clean surgical mask that covers the mouth and nose and is secured in a manner to prevent venting when open sterile supplies are present1 and when preparing, performing, or assisting with surgery and other invasive procedures, including
o â—‹ central venous catheter (CVC) insertion, peripherally inserted central catheters (PICCs), and guidewire exchange8″10;
o â—‹ regional anesthesia procedures11; or
o â—‹ high-risk spinal canal procedures (eg, myelogram, lumbar puncture, spinal anesthesia).10,12″20
[Recommended for Practice]
A clean surgical mask helps protect the patient and procedure site from microbial contamination by organisms carried in the provider»™s mouth or nose.1,3,10,21
Researchers studied the effectiveness of surgical masks in reducing the dispersal of bacterial contamination from the upper airways of 25 volunteers. The volunteers were asked to speak directly at an agar plate for five minutes. A surgical mask was applied and the volunteers were instructed to speak at the agar plate for three additional periods of five minutes each. The results showed a marked reduction in the bacterial contamination of the agar plates while the volunteers were wearing surgical masks.21
In a study investigating the possibility that surgical masks increase vertical shedding of bacteria from the face during facial movement, volunteers were asked to speak for 20 minutes while moving their heads from side to side without a surgical mask for the first five minutes and then with a surgical mask for three additional five-minute periods. A blood agar plate was positioned 30 cm below the volunteers»™ faces. The results showed a statistically significant reduction in the number of colony forming units on the agar plate when the volunteers were wearing surgical masks. The researchers recommended wearing a surgical mask, particularly when the perioperative team member»™s face is in close proximity to the procedural site and when the need for speaking during the procedure is anticipated.22
In a prospective, randomized, controlled trial of 221 patients, researchers assessed the need for surgical masks during cataract surgery. Patients were randomly assigned to group A, in which the surgeon wore a clean surgical mask, or group B, in which the surgeon did not wear a surgical mask. A settle plate was secured adjacent to the patient»™s head on the operative side within the sterile field during all procedures. The results showed a significant reduction of bacterial organisms falling on the operative side when the surgeon wore a surgical mask.23
In a study exploring the relationship between the use and position of a surgical mask during 30 cardiac catheterization procedures, researchers obtained bacterial samples within the draped, operative site adjacent to the femoral artery. Surgical masks were either not worn by perioperative team members, or worn in positions above and below the nose. The number of bacterial colonies recovered when no mask was worn was significantly greater than when a surgical mask was worn. Mask placement below the nose also was associated with a higher colony count than when the mask was worn above the nose. The researchers voluntarily discontinued the study after 30 patients in the interest of patient safety because of the high bacterial count associated with not wearing surgical masks.24
Surgical masks are effective in limiting the dispersal of oropharyngeal droplets21,25 and are recommended by the Centers for Disease Control and Prevention (CDC) for the placement of CVCs, PICCs, and guidewire exchange.8″10
The American Society of Regional Anesthesia and Pain Medicine recommends the use of surgical masks during regional anesthesia as a method to reduce the likelihood of site contamination from microorganisms that may be present in the upper airway of providers.11
Oropharyngeal flora was found to be the source of contamination in a number of reported cases of bacterial meningitis after lumbar puncture, spinal and epidural anesthesia, and intrathecal chemotherapy.12″19
In 2004, the CDC investigated eight instances in which patients contracted meningitis after procedures that involved placing a catheter or injecting material into the spinal canal or epidural space. The cases involved blood or cerebrospinal fluid contaminated with streptococcal species or other pathogens consistent with oropharyngeal fluid. None of the clinicians wore surgical masks during the procedures. Equipment and products used during these procedures were excluded as sources of contamination.10 In June 2007, the Healthcare Infection Control Practices Advisory Committee reviewed the cases and determined there was sufficient evidence to warrant the wearing of a surgical mask by the individual placing a catheter or injecting material into the spinal or epidural space.10
In September 2008, three cases of bacterial meningitis in postpartum women were reported to the New York State Department of Health. Two additional cases of meningitis were reported to the Ohio Department of Health in May 2009. All of the patients had received intrapartum spinal anesthesia. The investigators concluded that the New York incidents were associated with a single anesthesiologist. The anesthesiologist reported wearing a surgical mask; however, personnel reported that the presence of unmasked visitors in the procedure area was common. The Ohio incidents were found to be associated with a second anesthesiologist who did not wear a surgical mask. The findings underscore the need for adhering to aseptic practices and wearing surgical masks during spinal procedures.20
Perdonar la extensión del comentario y desde aquí todo mi respeto y apoyo a los profesionales que han realizado el artículo. Hay que seguir investigando y cualquier práctica está sometida a cambios.
Personalmente seguiré cumpliendo con las recomendaciones de la AORN, CDC, OMS y ASA.
Saludos a todos, cordialmente ARA.
Se agradece la respuesta, (aunque sea larga) pues el debate es el fin de esta plataforma.
Tal y como se ha comentado en la crítica del artículo, no queremos rebatir los protocolos y procedimientos que actualmente se disponen en torno a la mascarilla quirúrgica EN QUIRÓFANO FUERA DEL CAMPO QUIRíšRGICO y que se nos ofrecen con sus niveles de evidencia IV. Nuestro respeto también a los autores del artículo original, que un nivel de evidencia Ib parecen decir lo contrario, así como a los autores de la Cochrane que con su metaanálisis (evidencia Ia )también usan la duda como herramienta de conocimiento.
Aparte de las connotaciones médico legales que podría suponer no seguir las recomendaciones actuales en este tema, no debemos de olvidar, que parecen existir factores mucho más asociados a la tasa de infección de la herida postquirúrgica que la puesta o no de una mascarilla fuera del campo quirúrgico. Ese a sido nuestro propósito al escribir esta pequeña revisión crítica, así como poner la duda en el tema.
Interesante estudio. Sin ánimo de ser malo, y para que os riais un poco, os diré que las conclusiones me recuerdan un poco a esto:
<a href="http://www.ncbi.nlm.nih.gov/pmc/articles/PMC300808/pdf/32701459.pdf" rel="nofollow ugc">http://www.ncbi.nlm.nih.gov/pmc/articles/PMC300808/pdf/32701459.pdf</a>